
The time between eating and going to the bathroom can tell a lot about your health
It turns out that how quickly food passes through the intestines greatly affects the bacteria living there, and consequently, overall health. Scientists gathered data from dozens of studies and discovered that people with “fast” and “slow” digestion have noticeably different microbiomes. And this difference, apparently, is linked to a wide range of diseases, from chronic inflammation to Parkinson’s disease.
What Is Gut Transit Time
Gut transit time is the period it takes for eaten food to travel from the stomach to the exit of the large intestine. In Western countries, the norm is considered to be 30–40 hours, with an upper limit of about 70 hours. But in practice, the range is enormous: for some people, everything takes less than a day, while for others — more than three days.
It is precisely this time that determines how long gut bacteria are in contact with the contents of the large intestine. The longer food stays, the more time bacteria have for fermentation, pH regulation, and production of metabolites — substances that affect the health of the entire body.
Accumulated data indicates that gut transit time is a key factor shaping the composition and activity of the gut microbiota, which in turn is directly linked to human health. Nevertheless, when studying the microbiome, this parameter is still rarely taken into account.
What the Study on Digestion Speed Revealed
The scientific paper, published in 2023 in the peer-reviewed journal Gut, was a large-scale review — an analysis of existing scientific data rather than a separate experiment.
The team summarized the results of previously published studies, including data on participants’ transit times, stool consistency, diet, the composition of their microbiomes, and metabolites produced by gut microbes. In total, the review included studies involving thousands of patients, both healthy individuals and people with irritable bowel syndrome, chronic constipation, and liver cirrhosis.
It’s important to understand that this is not a clinical trial with specific conclusions like “do this — and you’ll be healthy.” This is an analytical review that systematizes what science already knows and shows where to go next.
How Digestion Speed Is Measured
Measuring transit time is not as simple as it might seem. Special swallowable capsules with sensors are used for this purpose, which record their journey through the digestive tract.
Another approach is the Bristol Stool Scale. This is a visual diagnostic scale developed at the Bristol Royal Infirmary in 1997 by Stephen Lewis and Ken Heaton. It classifies stool into seven types — from hard lumps (a sign of long transit) to liquid mush (a sign of fast transit). The authors of the scale concluded that stool form is a convenient indirect indicator of transit time.
Some studies track how long it takes participants to pass a swallowed blue dye or corn kernels. All these methods serve one purpose: to estimate how long food stays in the large intestine and how long bacteria have to interact with it.
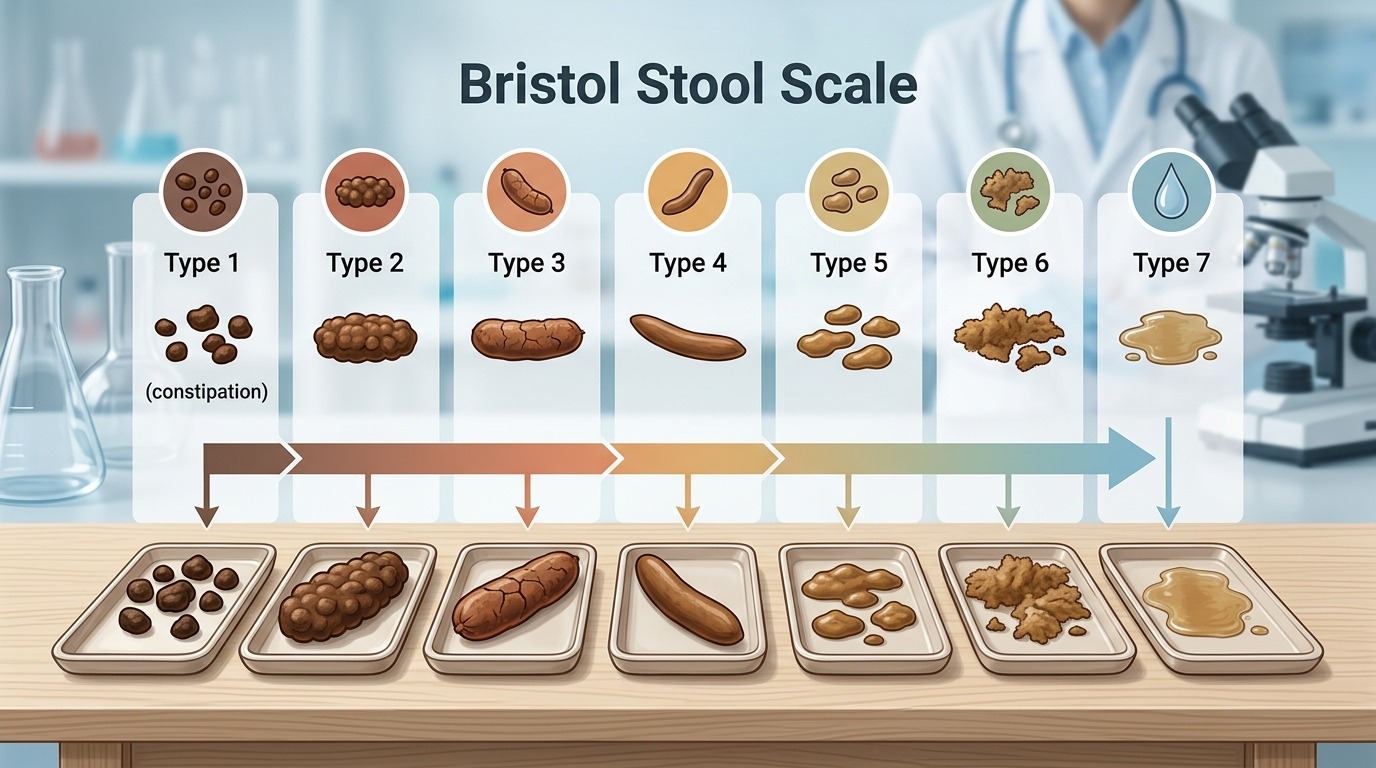
The Bristol Stool Scale helps assess digestion speed
How the Microbiome Differs with Fast and Slow Digestion
The review results were quite revealing. People with fast gut transit had a fundamentally different microbiome than people with slow transit. Moreover, adding transit time data to patient information allowed predicting microbiota composition more accurately than analyzing diet alone.
Here’s what the scientists found:
- People with fast transit had a microbiome populated predominantly by fast-growing bacterial species that prefer a diet high in carbohydrates and low in fats;
- With slow transit, species specializing in proteins dominated;
- Both “fast” and “slow” groups had lower microbiome diversity than people with average transit times. This means that extremes create an environment where highly specialized species prevail.
Then a feedback loop emerges: dominant bacteria release metabolites that maintain the existing status quo. Roughly speaking, if your gut is used to working slowly, its microbiome “tunes” itself to precisely this rhythm — and helps maintain it.
How Digestion Speed Is Linked to Parkinson’s Disease
Slow transit time and constipation are associated with metabolic and inflammatory disorders, as well as neurological diseases, particularly Parkinson’s disease. This connection is not coincidental: slowed gut transit and constipation are among the most common early symptoms of parkinsonism, which can appear years before the onset of motor disturbances.
Constipation affects more than 80% of patients with Parkinson’s disease and can precede motor symptoms by at least 10 years. This doesn’t mean that constipation causes Parkinson’s disease, but it points to a deep connection between gut health and the nervous system.
The microbiota produces metabolites: short-chain fatty acids, secondary bile acids, tryptamine, and histamine, which can stimulate gastrointestinal motility and thereby influence transit time. This once again confirms the bidirectional nature of the relationship: not only does gut speed affect microbes, but microbes also affect gut speed.
The connection between the gut and the brain is one of the most promising areas of neuroscience
Why Digestion Speed Matters for Treatment and Diet
One of the main practical takeaways of the review: two people can eat the same food and get completely different results, depending on how fast their gut usually works. This may explain why the same gut health recommendations don’t work for everyone.
Transit time may also affect the effectiveness of probiotics, supplements, and even medications that interact with the gut. Taking into account the individual digestive rhythm of a specific patient could help more precisely tailor diets and therapies.
As the review authors write, incorporating gut transit time measurements into microbiome research could advance the understanding of connections between microbiota, diet, and diseases. This knowledge could prove key for the prevention, diagnosis, and treatment of a whole range of illnesses.
It’s important to emphasize that for now, this is specifically a review of existing data, not ready-made clinical recommendations. The authors explicitly state that a deeper study of the complex bidirectional interactions between microbiota and transit time is necessary for a better understanding of microbiome variations in health and disease. But the approach itself — considering gut speed as a crucial rather than secondary parameter — could change how we study and treat diseases related to digestion.


