Fatty fish, eggs, and dairy products are natural sources of vitamin D
Vitamin D is called the “sunshine vitamin” and is considered almost a universal health booster. Interest in this vitamin surged especially during the coronavirus pandemic, as it was believed to protect against the disease. But there’s a flip side: excessive intake of vitamin D supplements can harm the body rather than strengthen it. Poisoning cases are rising worldwide, and doctors are increasingly reminding people: more does not mean better.
Why People Take Vitamin D
Vitamin D is not a single vitamin but an entire group of fat-soluble substances, the most important of which are D2 and D3. Approximately 90% of the necessary vitamin D is produced by the body itself when the skin is exposed to sunlight. The rest we get from food: fatty fish, egg yolks, and fortified dairy products.
The main role of vitamin D is to help the body absorb calcium and maintain bone strength. But its function doesn’t end there: it’s involved in immune system function, cell growth, metabolism, and neuromuscular activity. Long-term vitamin D deficiency is linked to an increased risk of neurological and autoimmune diseases, bone problems, and cardiovascular issues.
It’s precisely because of this wide range of effects that vitamin D has become one of the most popular supplements in the world. But popularity is no guarantee of safety, especially when it comes to high doses.
Excess Vitamin D: What Happens in the Body
When there’s too much vitamin D in the body, it excessively enhances calcium absorption from the intestines. As a result, blood calcium levels rise dangerously — a condition doctors call hypercalcemia. You can think of it this way: vitamin D is a “door” through which calcium passes from food into the blood. When there’s an excess of the vitamin, this door opens too wide, and calcium literally floods the bloodstream.
Excess calcium begins to deposit where it shouldn’t be: in artery walls, soft tissues, and — most dangerously — in the kidneys. This leads to a whole range of unpleasant symptoms:
- nausea and vomiting;
- constipation;
- severe fatigue and muscle weakness;
- bone pain;
- excessive thirst and frequent urination;
- kidney stones.
Most patients recover after discontinuing supplements and receiving treatment — usually intravenous fluids and medications to lower calcium levels are sufficient. But in rare cases, if the problem isn’t identified in time, vitamin D toxicity can lead to kidney failure requiring hemodialysis, and even life-threatening complications. There’s another alarming signal: some studies indicate that in elderly people, high blood levels of vitamin D may increase the risk of falls and injuries.
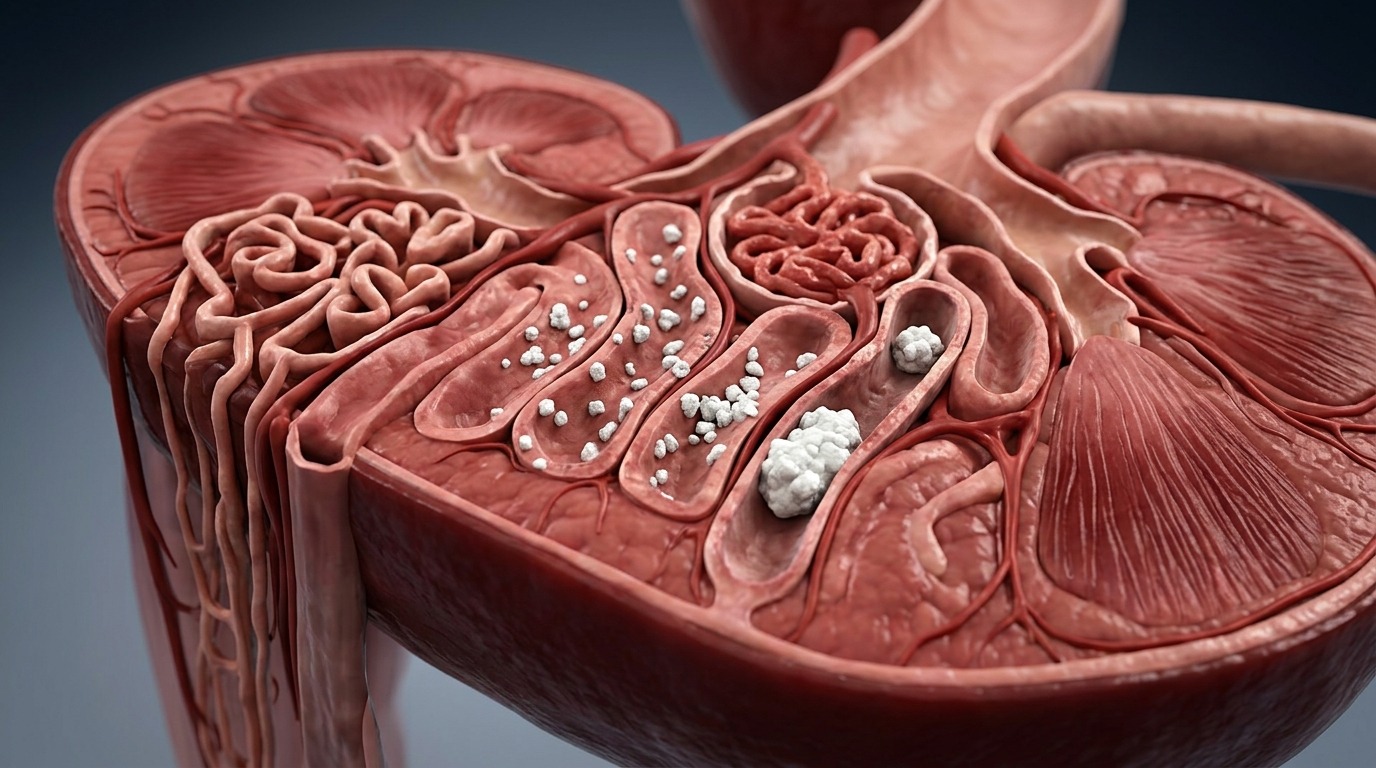
Excess calcium can lead to deposits forming in the kidneys
Vitamin D Poisonings Are Happening More Often
The problem isn’t the vitamin itself but how it’s taken. Vitamin D supplements are easily available over the counter today — in pharmacies, supermarkets, and online stores. Many formulas are unregulated, and dosages on packaging can be inflated.
The statistics speak for themselves. From 2000 to 2014, American poison control centers received more than 25,000 reports related to vitamin D intake. While from 2000 to 2005 an average of 196 cases were recorded per year, by 2011 that figure had risen by 1600% — to 4,535 reports annually. Among those affected were many children and adolescents. No fatalities were recorded during this period, but five cases resulted in serious medical consequences.
In 2018, scientists warned of “significant complacency” regarding the toxic effects of vitamin D. The authors linked the rise in poisonings to the popularity of books and media materials extolling high doses of this vitamin.
Errors in treating deficiency remain a separate problem. One documented case involved an 80-year-old man whose naturopath prescribed a weekly high-dose vitamin D tablet, but the patient mistakenly took it every day. Fortunately, after the error was corrected, his calcium levels returned to normal. And in 2016, Danish authorities were forced to recall a supplement from the market that contained 75 times the recommended dose of vitamin D, because about 20 children were harmed by it.

Vitamin D supplements are sold over the counter, and that’s not always a good thing
Safe Vitamin D Dosage
This is one of the most debated questions in modern nutrition science. Scientists still haven’t reached a consensus on exactly what dose of vitamin D becomes dangerous. But there are generally accepted guidelines.
Harvard Medical School specialists recommend: if you’re taking a vitamin D supplement, 600–800 IU (15–20 mcg) per day is likely sufficient. Without a doctor’s recommendation, you should not exceed 4,000 IU (100 mcg) per day, as this is considered the safe upper limit.
It’s important to understand that it’s virtually impossible to get vitamin D toxicity from sunlight or regular food — the body self-regulates how much vitamin the skin synthesizes. Problems begin specifically with supplements, especially high-dose formulas.
Harvard doctors also advise: if you have a vitamin D deficiency, it’s better to start with foods fortified with this vitamin rather than immediately reaching for pills — the risk of overdose with this approach is significantly lower.
Do Vitamin D Supplements Actually Help?
The scientific community is not unanimous on this point. Some studies show that vitamin D supplements may slow aging, improve cognitive function, or alleviate symptoms of depression. Other scientists question these results and believe that the real benefits of supplements are greatly exaggerated.
What is definitely known: vitamin D is critically important for health, but most people’s bodies are perfectly capable of getting it from sunlight and food. Mass supplement use “just in case,” without blood tests and a doctor’s prescription, is a practice that carries its own risks.

Before starting vitamin D supplementation, it’s worth checking your blood levels
Scientists emphasize that the decision to take vitamin D, especially in high doses, should be based on blood test results and a consultation with a doctor. This is not a case where “vitamins always mean something beneficial.”
Vitamin D is a perfect example of how important balance is. Its deficiency is truly dangerous and linked to a whole range of serious diseases. But uncontrolled supplement use can create a new problem instead of solving an old one. The best approach is to know your vitamin D level, not self-prescribe high doses, and remember that the most reliable source of this vitamin is still free — sunlight.


