
This small flower could save humanity, and that’s no exaggeration
A small yellow wildflower that has been used in folk medicine in Ireland and Europe for centuries has turned out to be capable of fighting bacteria resistant to modern antibiotics. A group of scientists published a study showing that the root extract of tormentil (Potentilla erecta) doesn’t just kill microbes — it enhances the effects of antibiotics and strips bacteria of their ability to build protective shelters. This is a very important discovery, especially considering that antibiotic-resistant bacteria can migrate throughout the body.
Why Antibiotics Are Losing Their Effectiveness
To understand why a humble flower from a bog suddenly became of interest to scientists, we need to grasp the scale of the problem. Antibiotic resistance is the ability of bacteria to survive despite drugs that used to destroy them. And the scale of this problem is frightening.
According to Science Alert, in 2023 every sixth laboratory-confirmed case of bacterial infection worldwide was characterized by antibiotic resistance. Between 2018 and 2023, bacterial resistance increased to 40% of the antibiotics being monitored. And the large-scale GRAM study predicts that without effective measures being taken, the total number of deaths associated with antimicrobial resistance worldwide will reach 39 million between 2025 and 2050.
Simply put, we risk returning to a time when an ordinary post-surgical infection or pneumonia once again becomes deadly. That’s exactly why scientists are searching for new ways to fight bacteria — and one of them was found in an unexpected place.
What Is Tormentil
Tormentil (Potentilla erecta) is an unassuming yellow flower that grows in bogs and meadows of Ireland, Great Britain, and continental Europe. The root of this plant has been used in Irish and European folk medicine for centuries: it was used to treat wounds, sore throats, diarrhea, and gum diseases.
This history of use hinted that perhaps there was something in this plant capable of killing microbes. And a team of scientists led by Professor Ronan McCarthy from the University of Southampton decided to systematically investigate this.
As part of a recent study published in the journal Microbiology, the team collected more than 70 plant species from Irish bogs, prepared extracts from them, and tested them in the laboratory against clinically significant bacteria — including those that cause severe pneumonia and urinary tract infections. Of all the candidates, tormentil extract showed the most notable antimicrobial effect.

Tormentil on an Irish bog — an unassuming flower with unexpected potential
How Tormentil Extract Kills Bacteria
The test results turned out to be very promising. The extract demonstrated two important properties: it suppressed bacterial growth and limited the formation of biofilms.
Biofilms are perhaps one of bacteria’s most unpleasant tricks. Imagine a bacterial community that surrounds itself with a slimy armor of polysaccharides. Bacteria inside biofilms can withstand antibiotic concentrations 100 and even 1,000 times higher than normal therapeutic doses. The antibiotic simply cannot break through this defense. That’s why biofilms are responsible for the majority of chronic infections that don’t respond to conventional treatment.
The fact that the extract of a humble bog flower can limit the formation of such protective structures is truly an important result. But the scientists didn’t stop there.
How Tormentil Extract Helps Antibiotics
A separate and perhaps the most intriguing part of the study was the attempt to combine the plant extract with existing antibiotics. The thing is, some plant compounds don’t kill bacteria directly but make antibiotics more effective — as if opening a door through which the medication then enters.
The scientists took the antibiotic colistin — a last-resort drug for treating infections caused by multidrug-resistant bacteria. Colistin is used only in extreme cases because it is toxic to the kidneys. At low doses, it couldn’t handle bacteria on its own. But when tormentil extract was added, the plant compounds significantly enhanced the antibiotic’s effectiveness.
This is fundamentally important. If a plant extract allows the use of lower doses of a toxic antibiotic while achieving better results, this could reduce side effects for patients. This approach is especially relevant for severe infections, from bacterial pneumonia to urinary tract infections, where superbugs are leaving doctors with fewer and fewer options.
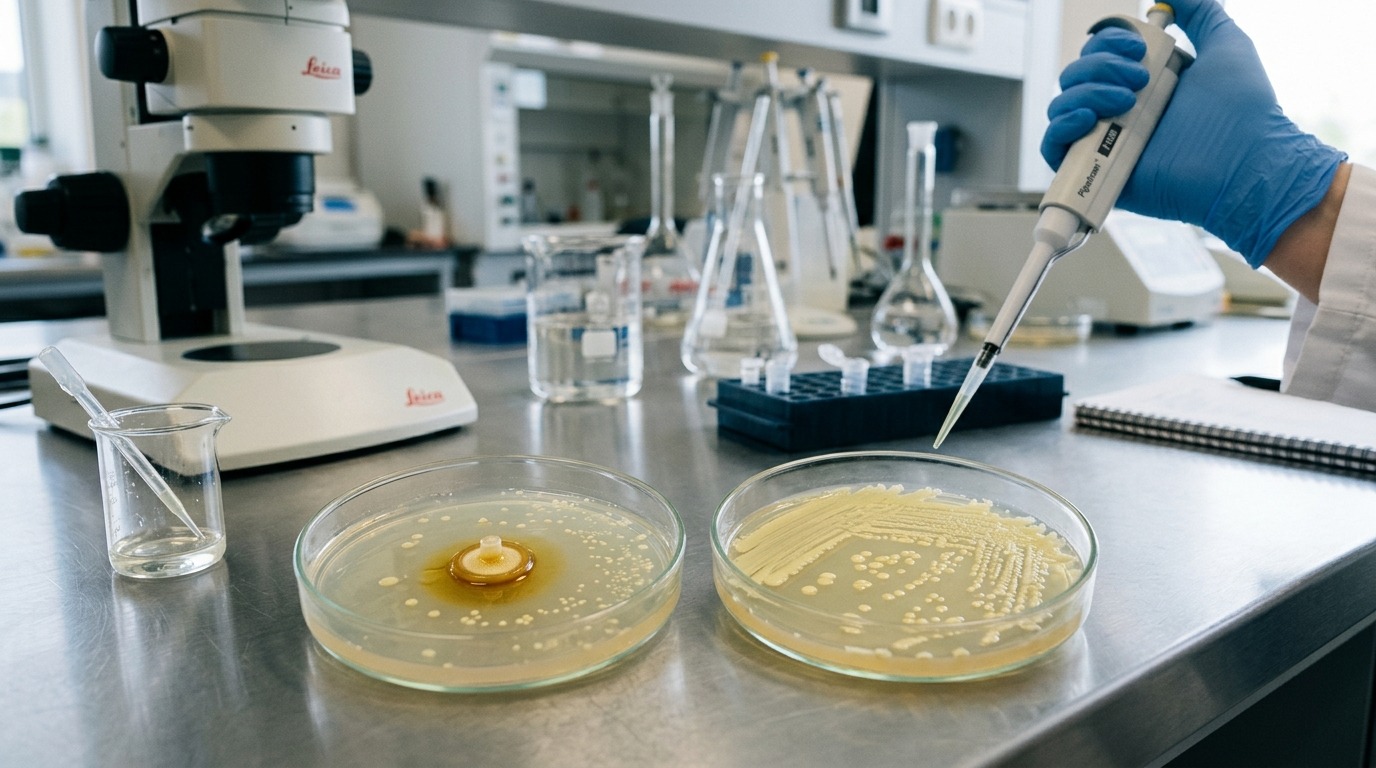
Laboratory Petri dishes with bacterial cultures: comparison of samples with and without the extract
How Tormentil Starves Bacteria of Nutrition
The researchers didn’t just document the effect — they figured out the mechanism. Analysis of the extract’s composition showed that two substances play a key role: ellagic acid and agrimoniin — natural compounds from the polyphenol group, known for their antioxidant and anti-inflammatory properties.
Tormentil root is exceptionally rich in polyphenols — tannins make up 20–25% of its dry mass. It was precisely these substances that turned out to be antimicrobially active.
The scientists discovered that these compounds work by “scavenging” iron from the bacteria’s environment. Iron is a critically important resource for bacteria, without which they cannot reproduce. Essentially, the plant molecules deprived bacterial cells of essential nutrition, preventing them from growing.
This is an elegant mechanism that is entirely different from most antibiotics. Conventional antibiotics destroy the bacterial cell wall, interfere with protein synthesis, or disrupt DNA. But here it’s a siege: the bacteria aren’t killed head-on — their supply lines are cut off. It’s harder for bacteria to develop resistance to this approach because the need for iron is their fundamental limitation.
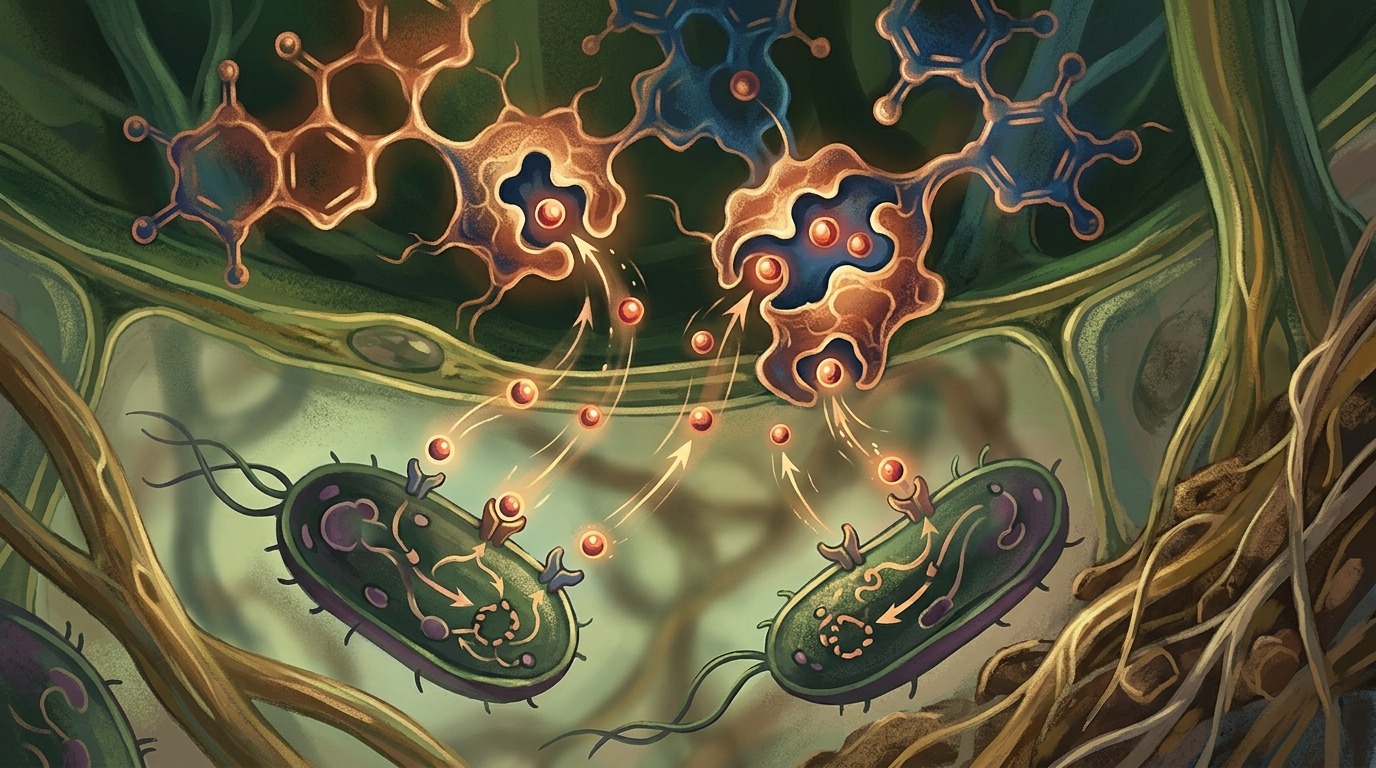
Schematic illustration of the mechanism: plant molecules intercept iron, depriving bacteria of a resource for growth
When to Expect a Tormentil-Based Medicine
It’s important to understand: this study was conducted in a laboratory, not on humans. Currently, the scientists are focused on optimizing antimicrobial activity and developing formulations for testing on experimental models. There is still a long way to go before clinical trials on patients.
The study of tormentil is not a ready-made medicine but a well-founded starting point. It demonstrates a specific mechanism of action, specific molecules, and a specific synergistic effect with an already existing antibiotic. This is far more than a vague claim that “folk medicine works.” And it reminds us that the answer to one of the greatest threats to modern medicine may literally be growing right under our feet.


