
As research has shown, bowel movement frequency reveals a lot about overall health. Image source: sciencealert.com
How often you have a bowel movement can reveal far more about your health than you might think. This is partly related to how your gut works and how quickly food passes through it. A large-scale study published in the journal Cell Reports Medicine showed that bowel movement frequency is closely linked to the health of the kidneys, liver, and gut microbiota. Moreover, the “sweet spot” turned out to be quite specific — once or twice a day.
What the Study Revealed About Bowel Movement Frequency in Adults
A team of scientists from the Institute for Systems Biology (ISB) in Seattle analyzed clinical, genetic, and microbiological data from 1,425 generally healthy adults — without chronic kidney or intestinal diseases. Participants self-reported how often they had bowel movements, and researchers cross-referenced this with their blood test results, stool samples, and detailed questionnaires about diet and lifestyle.
Bowel movement frequency was divided into four categories:
- Constipation — 1–2 times per week;
- Low-normal — 3–6 times per week;
- High-normal — 1–3 times per day;
- Diarrhea — 4 or more loose stools per day.
The scientists then looked for associations between these categories and a wide range of health indicators — from gut bacteria composition to blood plasma metabolites.
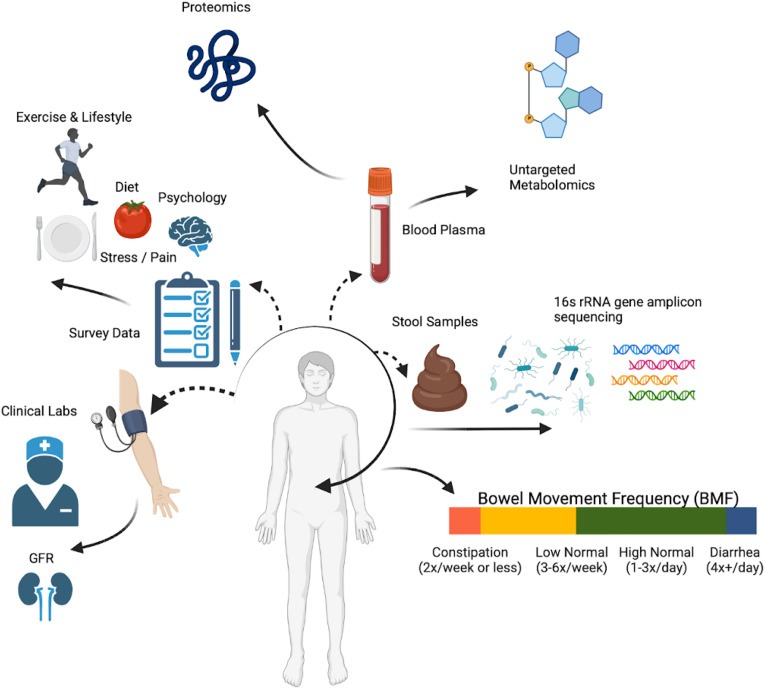
Study participants provided blood plasma and stool samples, and also filled out detailed questionnaires about their diet, health status, and lifestyle. Image source: cell.com
What Bowel Movement Frequency Is Considered Normal for a Healthy Person
The healthiest profile was found in people who had bowel movements once or twice a day. It was precisely in their guts that beneficial bacteria predominated — bacteria that feed on fiber and produce short-chain fatty acids, substances important for immunity, intestinal wall health, and overall metabolism.
The scientists called this optimal zone the “golden zone.” Participants in this group ate more fiber on average, drank more water, and engaged in physical activity more often.
Interestingly, demographic factors also influenced bowel movement frequency. Women, younger people, and participants with a lower body mass index tended to have fewer bowel movements on average. But even accounting for these differences, the association between extremes (constipation or diarrhea) and health problems remained consistent.
The Dangers of Constipation and What Happens in the Body With Infrequent Bowel Movements
Here’s what happens when stool remains in the intestines for too long. First, bacteria process all available fiber, converting it into beneficial short-chain fatty acids. But when the fiber runs out, microbes switch to an entirely different “fuel” — proteins. And the byproducts of protein fermentation are toxins.
Imagine a waste processing plant. As long as the right raw material (fiber) is fed in, the output is a useful product. But leave the system without fresh raw material, and it begins to break down whatever is available — with unpleasant byproducts.
Gut bacteria: when fiber is lacking, they switch to processing proteins.
This is exactly what blood tests confirmed. Participants with constipation had elevated levels of indoxyl sulfate in their blood — a toxic metabolite of bacterial protein processing that can damage the kidneys. Indoxyl sulfate is a well-studied substance: it causes oxidative stress in kidney tubule cells, triggers inflammation, and fibrosis — the replacement of normal tissue with scar tissue. Importantly, elevated levels of this toxin were found in people who had not yet received any diagnoses.
The Dangers of Diarrhea and How It Affects the Liver
On the other end of the spectrum, things aren’t smooth either. In participants with frequent loose stools, bacteria were found in the feces that normally inhabit the upper sections of the gastrointestinal tract — that is, the stomach and small intestine, rather than the large intestine where they belong. This indicates a disruption of normal microbial distribution.
And in the blood of these participants, biomarkers associated with liver damage and inflammation were elevated. The liver is a key organ for processing bile acids, which help digest fats. If the gut ecosystem is disrupted, this chain may not function as it should.
Thus, constipation and diarrhea affect different organs: constipation was more often associated with kidney risks, while diarrhea was linked to markers of liver damage. Notably, these were not sick individuals — all participants were considered healthy at the time of the study.
Constipation and diarrhea are associated with risks for different organs — kidneys and liver respectively.
How to Normalize Bowel Movements and Improve Gut Function
There is good news too. The gut microbiome is not something fixed once and for all. It can change, and quite rapidly. For example, a 2025 study from Germany showed that previously sedentary adults who began strength training 2–3 times a week saw noticeable changes in their gut bacteria composition within just eight weeks.
What helps you reach the “golden zone”:
- More fiber in your diet — vegetables, fruits, legumes, whole grains;
- Adequate water intake;
- Regular moderate physical activity — it supports peristalsis and helps the gut function more consistently.
However, it’s important to consider that everyone’s microbiome is unique. A 2025 study by American scientists showed that people with a higher abundance of methane-producing microbes in their gut are particularly efficient at converting fiber into beneficial short-chain fatty acids. This explains why two people on the same diet can have completely different outcomes. The microbiome is a kind of individual “filter” through which everything we eat passes.
Of course, everyone occasionally experiences constipation after a flight or diarrhea after a questionable street snack — that’s normal. But the study was specifically aimed at habitual, everyday rhythm — your “default mode.” And it turns out that this can point to hidden problems long before symptoms appear.
The study authors emphasize that the data obtained represent potential evidence of cause-and-effect relationships, not just correlations. However, further research is needed to confirm these findings.


