
Small blisters on the skin — a typical reaction in aquagenic urticaria
Imagine that every time after a shower, swimming in a pool, or even walking in the rain, itchy blisters appear on your skin. This is exactly what happened to a teenage girl whose case was described by Canadian doctors. The diagnosis turned out to be one of the rarest in dermatology — aquagenic urticaria, that is, an allergy to water.
The Rarest Type of Allergy
An allergy to water sounds like something incredible, because the human body itself is about 60% water. But aquagenic urticaria is a very real condition, first described back in 1964 by scientists Shelley and Rawnsley. When the skin comes into contact with water — of any temperature and from any source — the patient develops characteristic small blisters 1–3 mm in size, surrounded by redness. They usually appear on the upper body: neck, arms, torso, within 20–30 minutes and resolve within an hour or two after the skin dries. All of this was reported by the authors at Live Science.
But this is not a classic allergy in the usual sense. In a typical allergy, the immune system reacts to a specific protein — pollen, animal fur, nuts. Here, the trigger is water itself, regardless of whether it is tap water, distilled, or seawater. The exact mechanism has not yet been established, but there are several hypotheses.
According to one of them, water interacts with some substance in the skin or sebum, resulting in a compound that triggers the release of histamine — the very substance that causes swelling and itching in any allergic reaction. According to another theory, water dissolves an allergen hidden in the upper layers of the skin, and it penetrates deeper, activating immune cells.
What Water Allergy Looks Like
The case described in BMJ Case Reports by a group of Canadian scientists involves a teenage girl. Every time she took a shower, bath, or went swimming, blisters appeared on her skin — typical urticaria. The patient had no family history of such reactions, and she reported no systemic symptoms — no dizziness, shortness of breath, or wheezing.
Laboratory blood and urine tests showed that all major health indicators were normal. The girl had known allergies to dust, rabbits, and cats, but these allergens did not coincide with the episodes of urticaria after contact with water. Doctors needed to find the true cause, so they turned to a provocation test.
How to Know If You Have a Water Allergy
Diagnosing aquagenic urticaria is a puzzle in itself. The problem is that urticaria can be caused by pressure, cold, heat, physical exertion, and numerous allergens. Therefore, the doctor needs not only to see a reaction to water but also to rule out all other causes.
The standard method is the provocative water test. A damp cloth at a temperature of about 35 degrees is applied to the upper body of the patient for 20–30 minutes. If characteristic blisters appear on the skin, this is considered a positive result. It is important that the water is taken at room temperature or close to body temperature to avoid confusing the reaction with cold or heat urticaria. Additionally, tests for pressure, cold, and physical exertion are conducted to rule out other forms of physical urticaria.
In the case of the Canadian patient, a detailed medical history and a positive provocation test allowed doctors to confidently make the diagnosis — aquagenic urticaria.
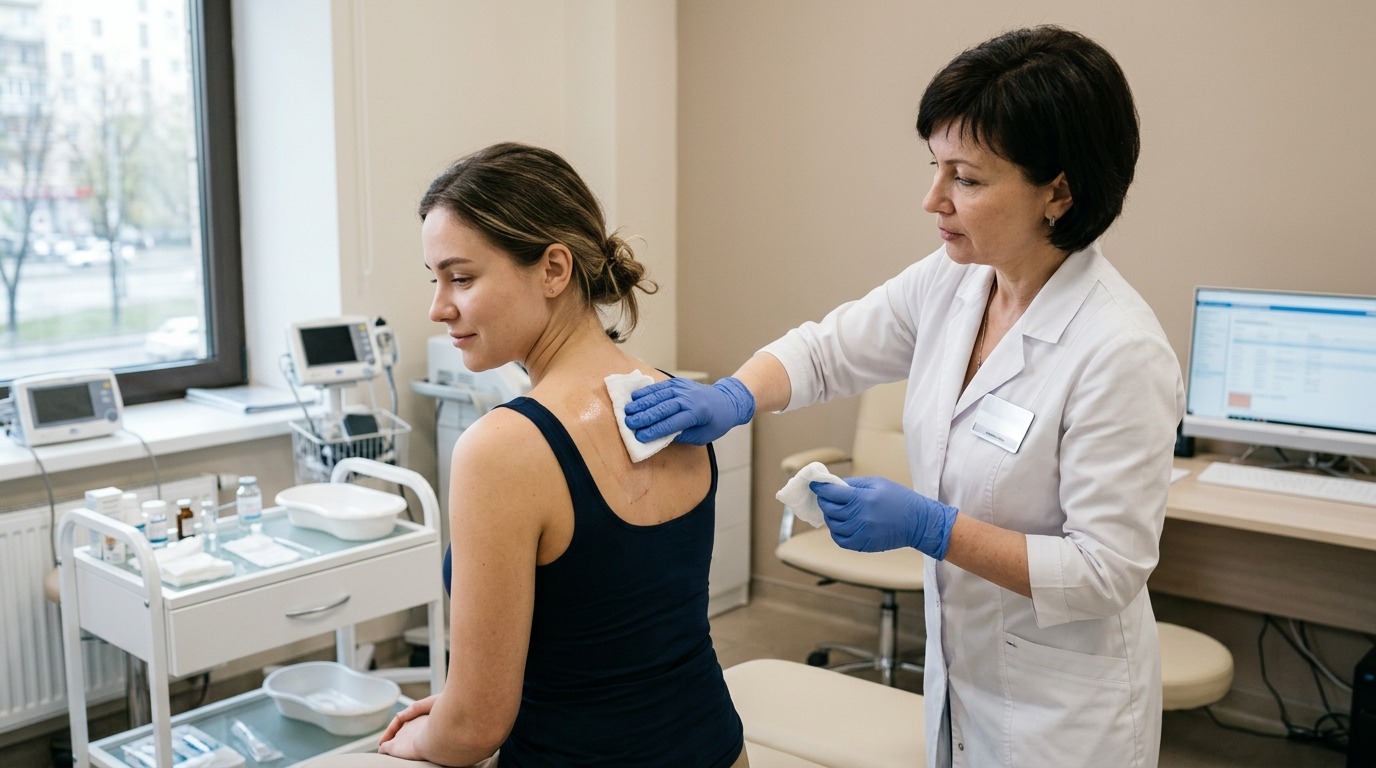
Provocation test: a damp cloth is applied to the skin and the reaction is observed
Symptoms of Water Allergy
Aquagenic urticaria typically first appears during puberty and is more common in women than in men. The main symptoms are:
- Small (1–3 mm) blisters, often with a red “halo” around them;
- Itching and discomfort in the area of the rash;
- Appearance of the rash within 20–30 minutes after contact with water;
- Predominantly located on the arms, neck, chest, and back;
- Spontaneous disappearance of blisters within 30–60 minutes after the skin dries.
Anything can trigger a reaction: a shower, bath, pool, rain, sweat, and even tears. Severe systemic reactions — shortness of breath, wheezing, throat swelling — are very rare. Most patients experience only skin manifestations, which, however, already creates enormous psychological discomfort: people find it difficult to take showers, exercise, and lead a normal life.

Even ordinary rain can be a problem for people with aquagenic urticaria
How Water Allergy Is Treated
Completely avoiding contact with water is impossible, so treatment is aimed at controlling symptoms and allowing the person to live normally. The main line of therapy is second-generation antihistamine medications. They block the action of histamine and help prevent or reduce rashes.
The Canadian patient received one of these medications, and the results were good: after 14 months of follow-up, she reported living a normal life without any restrictions, provided she continued taking the medication. However, other patients may respond differently to antihistamines.
It is important to understand that remission in aquagenic urticaria occurs unpredictably. Some patients live with this condition for decades. But with proper selection of therapy, most maintain a normal quality of life.
Why the Causes of Water Allergy Are Unknown
To date, fewer than 100 cases of aquagenic urticaria have been described in the world medical literature. A 2022 systematic review found data on only 77 patients from 59 studies. This makes water urticaria one of the least studied types of chronic urticaria. Due to this rarity, neither the cause of the disease, nor its prevalence, nor the likelihood of remission have been precisely established.
Each newly described case is a chance to better understand what exactly happens in the skin upon contact with water. Researchers hope that studying the skin barrier will help uncover the mechanism of the disease and find more precise treatment methods. For now, aquagenic urticaria remains a rare but very real condition that turns the most common substance on Earth into a source of discomfort.


