Barry Marshall ate dangerous bacteria to prove the effectiveness of a new method for treating stomach ulcers
In medicine, there is an unspoken rule: don’t question what works. Especially if it is backed by decades of practice, thousands of surgeons, and millions of operated patients. But in the early 1980s, one Australian doctor did exactly that, and his discovery literally turned gastroenterology upside down, while simultaneously angering the surgical community worldwide.
Gastroenterology is a branch of medicine that deals with the study, diagnosis, treatment, and prevention of diseases related to the gastrointestinal tract (GIT).
How Stomach Ulcers Were Treated Before the Discovery of the Bacterium
Peptic ulcer disease of the stomach and duodenum was for many decades considered the result of stress, poor diet, and excessive acidity. The logic was simple: acid erodes the stomach wall, so you either need to reduce acidity or remove the part of the stomach that produces it. Surgeons around the world performed a procedure called vagotomy — an operation in which the branches of the vagus nerve that stimulate hydrochloric acid production were severed. In severe cases, patients had up to two-thirds of their stomach removed (gastrectomy).
And these were not isolated cases. By the early 1980s, gastrectomy and vagotomy were among the most common elective surgeries in the world. Surgeons built careers on this, wrote dissertations, and trained students. The operation was considered the gold standard for ulcer treatment. Patients often suffered from digestive problems for the rest of their lives afterward, but there seemed to be no alternative. Medications and diets provided only temporary relief, and ulcers kept coming back again and again.
For comparison: today, stomach ulcers are treated with a course of antibiotics over one to two weeks. But it took a real war in medicine to arrive at this simple solution.
Who Is Barry Marshall and What He Found in the Stomach
In 1981, a young Australian intern named Barry Marshall began working at the Royal Perth Hospital under the supervision of pathologist Robin Warren. By that point, Warren had already been observing a strange pattern for several years: in gastric mucosal biopsies from patients with gastritis and ulcers, he repeatedly found spiral-shaped bacteria. The problem was that according to textbooks, bacteria could not survive in the stomach — hydrochloric acid was considered an insurmountable barrier.

Barry Marshall and Robin Warren. Image source: Live Science
Marshall became interested in Warren’s findings and began a systematic investigation. Together, they studied biopsies from over a hundred patients and found a clear correlation: the bacterium, which would later be named Helicobacter pylori, was present in nearly all patients with ulcers. It turned out that this microorganism hides under the mucus layer protecting the stomach wall and produces an enzyme called urease, which neutralizes the acid around it. In simple terms, the bacterium created its own comfortable habitat in the most aggressive environment in the body.
In 1983, Marshall and Warren presented their initial results. The response from the medical community was, to put it mildly, cold.
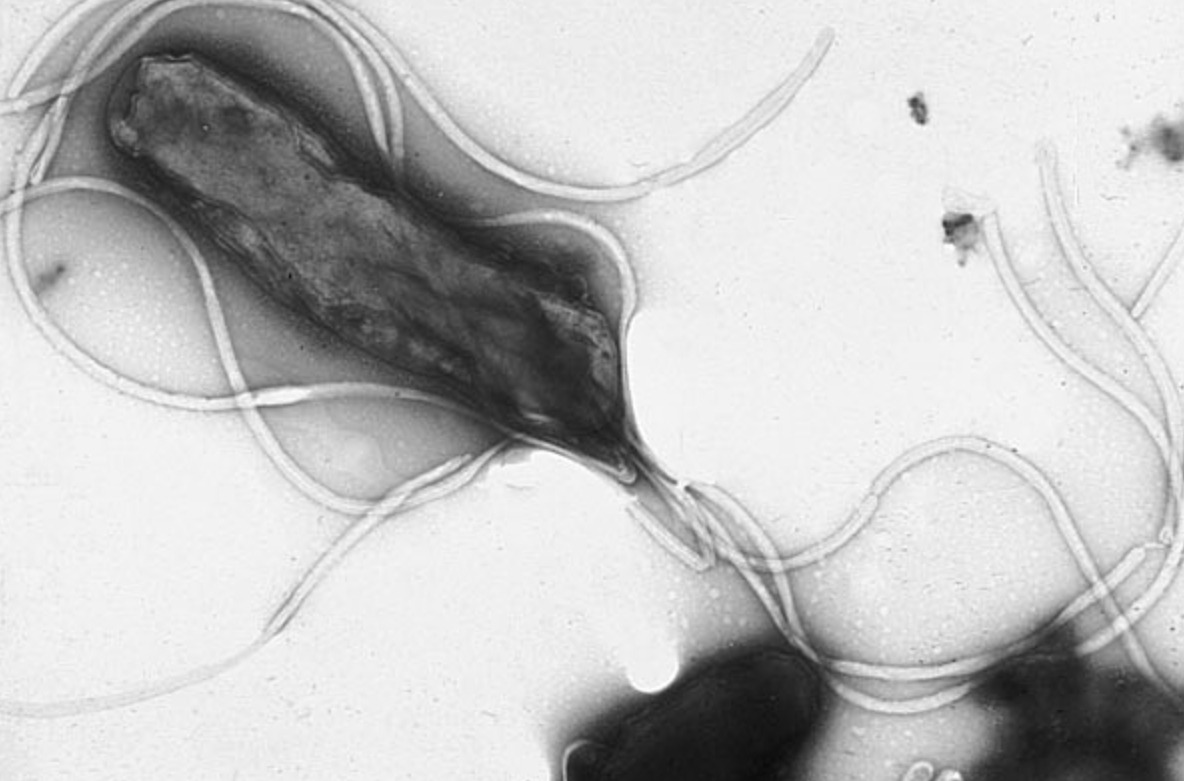
The bacterium Helicobacter pylori under a microscope. Image source: wikimedia.org
Why Surgeons Did Not Believe in the Bacterial Nature of Ulcers
This is where the most dramatic part of the story begins. When Marshall claimed that ulcers are caused by a bacterium, not stress, and that they should be treated with antibiotics rather than a scalpel, the reaction was predictable. They simply didn’t believe him.
There were several reasons. First, decades of an established paradigm. Textbooks, monographs, clinical guidelines — everything pointed to acid and stress. Second, the economic factor: surgical treatment of ulcers was a massive industry. Operations brought hospitals and surgeons a steady income. Third, Marshall himself was young and had no significant scientific standing. At one conference where he presented his results, someone in the audience asked the now-legendary question:
Are you saying I’ve been cutting out people’s stomachs for nothing?
The thing is, acknowledging Marshall’s correctness would mean admitting that thousands of patients had undergone disfiguring operations unnecessarily. That decades of surgical practice had been a mistake. That an entire generation of doctors had been treating the consequence, not the cause. For the medical community, this was quite a test.
Marshall was ridiculed at conferences, and his papers were rejected by reviewers. One of the leading gastroenterologists of the time publicly called his hypothesis “the ravings of a madman.”
How Barry Marshall Drank Bacteria and Proved Himself Right
By 1984, Marshall’s patience had run out. He was not allowed to conduct a full clinical trial on humans — the ethics committee would not approve the experiment. So Marshall made a decision that would go down in medical history: he drank a culture of Helicobacter pylori himself.
The result came quickly. Within a few days, he developed acute gastritis with nausea, vomiting, and abdominal pain. A biopsy confirmed that the gastric mucosa was inflamed and that the bacteria were actively colonizing its surface. Marshall then completed a course of antibiotics and fully recovered within two weeks.
But even after that, recognition did not come immediately. It took nearly another decade of large-scale research before, in 1994, the U.S. National Institutes of Health officially recognized that most stomach and duodenal ulcers are caused by Helicobacter pylori and should be treated with antibiotics. The number of surgeries to remove parts of the stomach dropped dramatically after that.
And in 2005, Barry Marshall and Robin Warren received the Nobel Prize in Physiology or Medicine. More than twenty years had passed from the moment of discovery to recognition.

Barry Marshall and Robin Warren receiving the Nobel Prize. Image source: Reuters
What the Story of the Helicobacter pylori Discovery Teaches Us
The story of Marshall and Warren is often cited as an example of how conservative medicine can be. But it would be unfair to accuse surgeons of malicious intent. They were acting within the paradigm of their time and saving lives with the tools they had. The problem was not with individual doctors, but with a system that was too slow to revise established dogmas.
Today, Helicobacter pylori is found in approximately half of the world’s population, although far from all carriers develop ulcers. Diagnosis uses a simple breath test, and standard therapy includes a combination of two antibiotics and medications to reduce hydrochloric acid. Treatment lasts from 7 to 14 days, and in most cases, the ulcer never returns.
But here’s what’s important: this story is not just about a bacterium. It’s about how one stubborn doctor, willing to risk his own health, changed the fate of millions of patients. And about how in science, the most dangerous enemy of progress is not ignorance, but the illusion of knowledge.
Marshall’s case reminds us that if someone in a white coat says something uncomfortable, it doesn’t mean they’re wrong. Sometimes the most important discoveries begin with a phrase that nobody wants to hear.


