
Capgras syndrome reminds us of the fragility of perception: what we take for granted is held together by invisible threads of neural connections
Some people one day realize with horror that their loved ones have become strangers to them. The face is the same, the voice is the same, but something inside screams: that’s not them. Capgras syndrome is a rare psychiatric disorder in which a person genuinely believes that their loved ones have been replaced by impostors. And this is not a horror movie plot, but a real diagnosis with very specific causes.
What Is Capgras Syndrome and How Does It Manifest
The syndrome was named after French psychiatrist Joseph Capgras, who in 1923 described the case of a patient named Madame M. The woman was convinced that her husband, children, and even neighbors had been replaced by identical copies — “doubles.” She felt no usual warmth toward them and treated them with suspicion, even though these people looked no different from those she had known her entire life.
The main feature of the syndrome is delusional misidentification. The patient visually recognizes the person, but the emotional connection to them is completely severed. Simply put, the brain sees a familiar face but feels nothing. And instead of attributing this to fatigue or stress, the mind finds a “logical” explanation: this person has been replaced.
Sometimes the delusion extends beyond people. There are known cases where patients believed their pets, their home, and even their personal belongings had been replaced. Everything around becomes a stage set — like a bad play where actors carefully copy familiar people, but the falseness is still noticeable.

Jean Marie Joseph Capgras. Image source: new-science.ru
Why the Brain Stops Recognizing Loved Ones
At first glance, it seems like the problem lies in vision or memory. But in reality, the mechanism is far more subtle. The thing is, face recognition is a two-step process. First, the visual cortex processes the image and determines: “Yes, this is Masha’s face.” Then the limbic system, the brain’s emotional center, adds a feeling to this image: warmth, attachment, trust.
In patients with Capgras syndrome, the first step works perfectly, but the second one breaks down. Neurobiologists believe the cause lies in a disrupted connection between the fusiform gyrus (responsible for face recognition) and the amygdala (which processes emotions). When this “bridge” is destroyed, the face of a loved one evokes not love, but an unsettling emptiness.
It turns out that confirmation of this theory was obtained in experiments measuring galvanic skin response. When a healthy person is shown a photograph of a relative, their body reacts slightly: palms sweat, pulse quickens. In patients with Capgras syndrome, this response is completely absent when looking at loved ones, although everything works normally when seeing strangers.
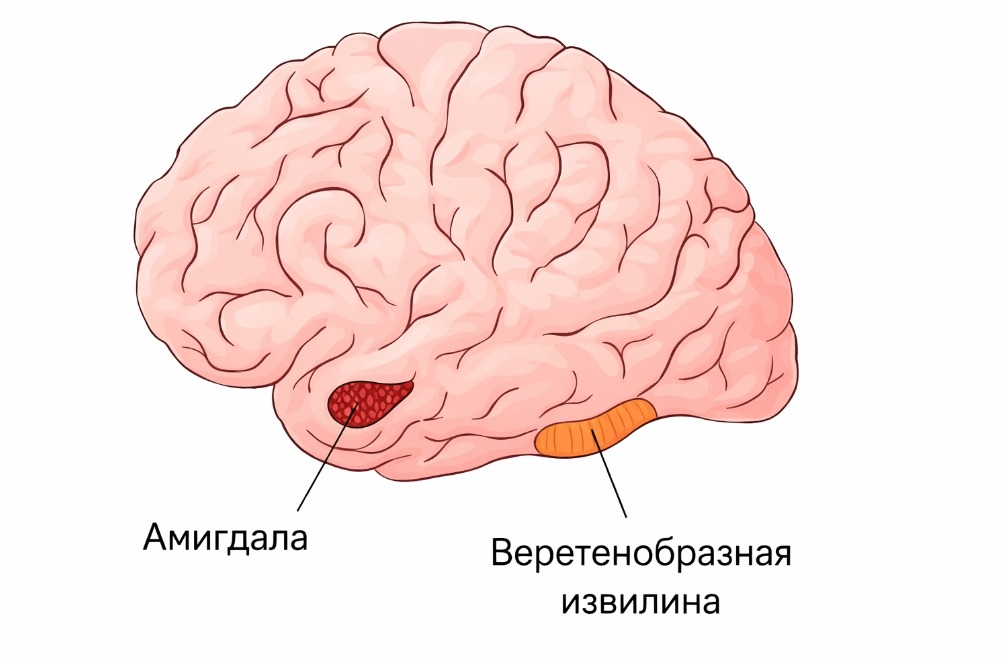
Amygdala and fusiform gyrus
What Diseases Cause Capgras Syndrome
Capgras syndrome is not a standalone disease but rather a symptom that arises against the background of other disorders. Most commonly, it accompanies neurodegenerative diseases. According to statistics, up to 16% of people with Alzheimer’s disease and about 17% of people with Lewy body dementia experience this delusion.
But that’s not all. The syndrome is found in schizophrenia, epilepsy, traumatic brain injuries, and even after strokes. Sometimes it manifests in patients with vitamin B12 deficiency or against the background of hypothyroidism. In other words, any serious damage to the brain’s “emotional wiring” can trigger this mechanism.
Interestingly, Capgras syndrome often co-occurs with other delusional disorders. For example, with Fregoli syndrome — when the patient, on the contrary, is convinced that different people around them are the same person in disguises. Or with Cotard syndrome, in which the patient believes they are dead. A brain that has lost its usual reference points can generate the most bizarre explanations of reality.
How Capgras Syndrome Is Treated and Whether the Patient Can Be Helped
Unfortunately, there is no magic pill for Capgras syndrome. Treatment is primarily aimed at the underlying disease that triggered the delusion. If it’s schizophrenia, antipsychotic medications are prescribed. If it’s dementia, cholinesterase inhibitors are used to slow the destruction of neural connections.
However, working with the patient’s environment is equally important. Specialists recommend that relatives not argue or try to convince the patient otherwise. Phrases like “But it’s me, your wife!” don’t help — they only increase anxiety. It is much more effective to gently redirect attention, create a calm environment, and consult a doctor.
There are also encouraging cases. Medical literature describes situations where, after successful treatment of the underlying disease or recovery from injury, Capgras syndrome receded. The brain restored its lost connections, and loved ones became “their own” again. But the path to this is long and requires patience from everyone.

The most important thing loved ones can do is not take offense and remember that what they’re facing is not cruelty, but illness. Image source: IFL Science
How Capgras Syndrome Differs from Memory Loss
Many people confuse Capgras syndrome with amnesia or prosopagnosia — the inability to recognize faces. But the difference is fundamental. With prosopagnosia, a person truly cannot recognize a face — neither visually nor emotionally. With amnesia, they forget people entirely. But with Capgras syndrome, the patient sees and remembers perfectly well, yet feels nothing.
This makes the disorder especially agonizing for those around the patient. The person doesn’t just fail to recognize you — they actively reject you. They may become hostile, fearful, and sometimes even aggressive toward the “impostor.” For families, this is a true ordeal: the person you love looks at you as a threat.
Neurobiologists emphasize that Capgras syndrome is a window into understanding how our brain constructs reality. We are accustomed to thinking that “seeing is believing.” But it turns out that without an emotional underpinning, vision alone does not provide a sense of authenticity. Our brain doesn’t just see the world — it feels it. And when the feelings are switched off, reality falls apart.
Capgras syndrome is not a whim or a fabrication. It is a serious disorder behind which lies damage to the brain’s most delicate mechanisms. And perhaps the main lesson it teaches is this: to recognize a person means not only seeing their face but also feeling their presence. When science learns to reliably restore this connection, many people will regain those they “lost” — even without ever being apart from them.


